 28
Feb,2026
28
Feb,2026
Swimmer’s ear isn’t just a nuisance-it’s a real infection that can turn a fun day at the pool into days of pain and frustration. Unlike middle ear infections, which happen behind the eardrum, otitis externa attacks the skin lining your ear canal. It’s common, especially in warm, humid places like Melbourne, where people swim often and sweat heavily. The good news? Most cases clear up fast with the right treatment. The bad news? Many people waste time trying home remedies or using the wrong ear drops, making it worse.
What Really Causes Swimmer’s Ear?
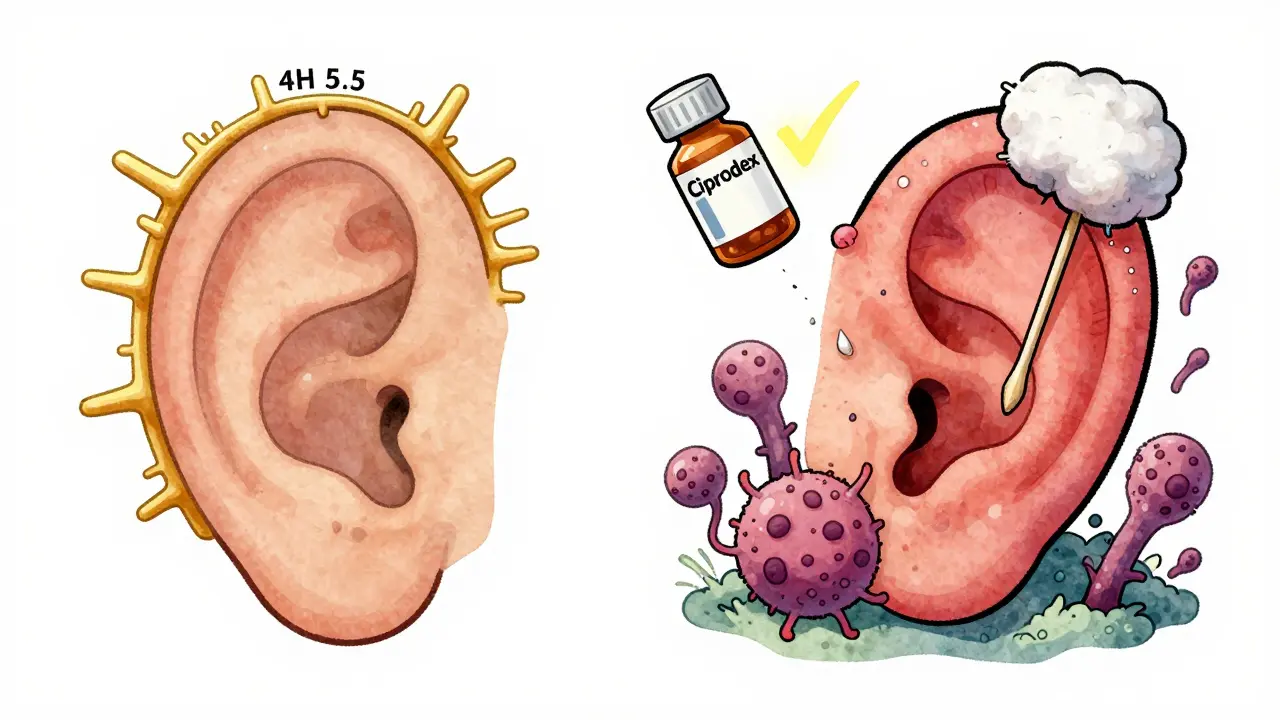
It’s not just water. While swimming is the most common trigger, any moisture trapped in the ear canal can set the stage for infection. Showering, sweating, or even using cotton swabs can disturb the ear’s natural defenses. The ear canal normally has a slightly acidic pH between 5.0 and 5.7, thanks to earwax. This acidity keeps bacteria and fungi in check. When water washes away that protective layer, pathogens move in.The two biggest culprits are bacteria: Pseudomonas aeruginosa (responsible for over half of cases) and Staphylococcus aureus. Fungi like Aspergillus cause about 1 in 10 cases, especially after prolonged antibiotic use. People with diabetes or eczema are at higher risk because their skin heals slower and resists infection less effectively.
Here’s what actually leads to infection:
- Swimming in contaminated water (pools, lakes, hot tubs)
- Using cotton swabs, bobby pins, or earbuds that scratch the canal
- Living in humid climates where moisture lingers
- Having narrow ear canals (common in kids)
- Wearing hearing aids or earplugs that trap moisture
How Bad Is It? Recognizing the Levels
Not all swimmer’s ear is the same. It comes in three stages, and knowing which one you have determines what treatment you need.- Mild (45% of cases): Itchy, slightly red ear canal. Minor discomfort when tugging the earlobe. No swelling blocking the canal.
- Moderate (35%): More pain, noticeable swelling, partial blockage of the ear canal. Hearing might feel muffled.
- Severe (20%): Intense pain, even when not touching the ear. Complete canal blockage from swelling. Fever over 38.3°C. Swollen lymph nodes near the neck.
If you have a fever or the pain is spreading to your face or neck, don’t wait. See a doctor immediately. In rare cases (0.03%), it can turn into malignant otitis externa-a dangerous infection that spreads to bone and cartilage, mostly in diabetics or older adults.
What Ear Drops Actually Work?
Treatment isn’t one-size-fits-all. The right drop depends on whether it’s bacterial or fungal, and how bad it is.For mild cases: Over-the-counter 2% acetic acid with hydrocortisone (like VoSoL HC Otic or Swim-Ear) works wonders. It restores the ear’s natural acidity and reduces inflammation. Studies show it clears up symptoms in 85% of mild cases within a week. It’s cheap-around $15 for a bottle-and safe to use after swimming as a preventive measure. Users on Amazon give it 4.1 out of 5 stars, mostly because it stops infections before they start.
For moderate to severe cases: Prescription drops are necessary. The gold standard is ciprofloxacin 0.3% with dexamethasone 0.1% (brand name Ciprodex). This combo kills bacteria and reduces swelling fast. Clinical trials show 92% of patients are symptom-free in 7 days. It’s more expensive-about $147.50 without insurance-but worth it if you’re in pain. A 2020 NEJM study found it works better than antibiotic-only drops.
There’s also a newer option: ofloxacin otic solution (OtiRx), approved by the FDA in March 2023. It’s an extended-release formula that lasts 24 hours instead of 12, meaning fewer doses. Early trials show 94% effectiveness, and it’s already being used in clinics in Australia and the U.S.
For fungal infections (otomycosis): Acetic acid won’t cut it. You need antifungals. Clotrimazole 1% solution works in 93% of cases, according to a 2021 JAMA Otolaryngology study. It’s usually prescribed as drops or a cream applied daily for 7-10 days.
Why Some Drops Fail (and What to Avoid)
Not all ear drops are equal. Some are outdated-or even dangerous.Avoid aminoglycosides like neomycin or polymyxin B. They’re cheaper (around $25 per bottle) and still sold in some OTC products. But they carry a 5-7% risk of causing allergic skin reactions, and worse-they’re ototoxic. If your eardrum is perforated (even a tiny hole), these drops can damage your hearing permanently. The FDA warns against them for this reason.
Also, don’t use antibiotic drops if you have a fungal infection. You’ll just make it worse. Many people self-treat with Ciprodex when they have a fungal infection, and it delays real treatment by 7-10 days. That’s why 15% of emergency visits for worsening ear infections involve people who used the wrong drops.
How to Use Ear Drops Right
Even the best drops won’t work if you use them wrong. Here’s what actually helps:- Wipe the outer ear with a dry cloth-never stick anything inside the canal.
- Warm the bottle in your hands for 1-2 minutes. Cold drops can cause dizziness.
- Lie on your side with the infected ear facing up.
- Put in the number of drops prescribed (usually 5).
- Stay lying down for 5 full minutes. This lets the medicine reach deep into the canal.
- Then, sit up slowly. Let the excess drain out. Don’t plug it with cotton.
Skipping the 5-minute wait reduces effectiveness by 40%. That’s according to Mayo Clinic data. And never use cotton swabs after applying drops-they’ll suck out the medicine.
When You Need More Than Drops
If your ear canal is swollen shut, drops alone won’t reach the infection. In those cases, a doctor will insert an ear wick-a tiny, sponge-like strip that absorbs the drops and slowly releases them into the blocked area. About 65% of patients say it’s uncomfortable, but 90% say it’s worth it. Without it, treatment fails.Also, if you’re diabetic, have a weakened immune system, or if symptoms don’t improve in 3-4 days, see a specialist. You might need oral antibiotics or a deeper cleaning under an otoscope.

Prevention Is Easier Than Treatment
The best treatment is avoiding it altogether. Here’s how:- After swimming or showering, tilt your head to drain water. Gently pull the earlobe to help it flow out.
- Use a hairdryer on low heat, held at arm’s length, to dry the ear.
- Use a few drops of 2% acetic acid solution after swimming-it cuts recurrence risk by 65%.
- Never use cotton swabs, bobby pins, or anything sharp inside the ear.
- Wear well-fitting earplugs designed for swimming, not regular foam ones.
Studies show people who use preventive drops after swimming cut their risk of infection by more than half. It’s simple, cheap, and effective.
What’s New in Treatment?
The field is evolving. Researchers at Stanford are testing microbiome-based treatments-drops that restore the ear’s natural bacterial balance instead of killing everything. Early trials are promising. Meanwhile, telemedicine is making diagnosis easier. Mayo Clinic’s 2022 pilot found video calls correctly diagnosed swimmer’s ear 88% of the time.But the biggest threat? Antibiotic resistance. Between 2015 and 2020, fluoroquinolone-resistant Pseudomonas strains increased by 12%. That’s why experts like Dr. Michael H. Mison warn against overprescribing. Use drops only when necessary.
Final Takeaway
Swimmer’s ear is common, treatable, and preventable. Mild cases? Try OTC acetic acid drops. Moderate to severe? See a doctor for Ciprodex or OtiRx. Fungal? Use clotrimazole. Never use cotton swabs. Always follow the 5-minute rule. And if you’re diabetic or have recurring infections, don’t ignore it-get checked early.The bottom line: You don’t need to quit swimming. You just need to protect your ears.
Can I use hydrogen peroxide to clean my ear if I have swimmer’s ear?
No. Hydrogen peroxide can irritate the ear canal and damage the skin, making the infection worse. It doesn’t kill the bacteria causing swimmer’s ear and can delay healing. Stick to prescribed drops or OTC acetic acid solutions. Never put anything inside the ear canal unless directed by a doctor.
Why do my ears hurt more at night?
Pain often worsens at night because lying down increases pressure on the ear canal, and there’s less distraction from the pain. Also, your body’s natural anti-inflammatory response is lower at night. If pain wakes you up, it’s a sign the infection is moderate to severe-see a doctor.
Can children get swimmer’s ear too?
Yes. Children aged 7-12 have the highest incidence rate-14.2 cases per 100 kids each year. Their ear canals are narrower, and they often swim more. Use child-safe drops like acetic acid solutions. Never use adult prescription drops without a pediatrician’s advice. Always keep their ears dry after swimming.
Is it safe to use ear drops if I have a perforated eardrum?
Only if the drops are specifically labeled as safe for perforated eardrums. Fluoroquinolones like ciprofloxacin and ofloxacin are generally safe. But aminoglycosides like neomycin are ototoxic and can cause permanent hearing loss. Always tell your doctor if you’ve had ear surgery or a ruptured eardrum in the past.
How long should I use ear drops before seeing a doctor?
If you’re using OTC drops and see no improvement in 3 days, or if pain worsens, see a doctor. Prescription drops should start working in 24-48 hours. If you still have pain, swelling, or fever after 5 days, you may need a different treatment or further testing for fungal infection or complications.
Can I swim while being treated for swimmer’s ear?
Avoid swimming until symptoms are gone. Water reintroduces bacteria and delays healing. If you must swim, use waterproof earplugs and apply a few drops of acetic acid solution immediately after. Dry your ears thoroughly afterward. Most doctors recommend waiting 7-10 days after symptoms disappear before returning to regular swimming.




Let me tell you something about swimmer’s ear that no one talks about-it’s not just about water. It’s about how modern life has turned our bodies into fragile, over-sanitized ecosystems. We shower with antibacterial soap, wear noise-canceling earbuds for hours, and then wonder why our ear canals turn into petri dishes. The ear isn’t a hole to be cleaned-it’s a living ecosystem. When you disrupt its pH with cotton swabs or hydrogen peroxide, you’re not removing dirt-you’re committing ecological sabotage. And yet, we keep doing it because we’ve been lied to by commercials that sell ‘deep cleaning’ as self-care. The real solution? Let the ear do its job. A little wax. A little acidity. A little silence.
Just used VoSoL HC after a pool day. No issues. Do the 5-minute lie-down. It works.
I’m from Texas and my grandma used to rub a drop of olive oil in her ear after swimming. I thought it was an old wives’ tale-until I tried it last summer. Not a single infection. I still use it. Not a cure, but a shield. Maybe it’s the fatty acids? Or maybe it’s just the ritual. Either way, it works for me.
Yeah right, ‘Ciprodex’ works. I’ve been to three doctors in Melbourne and each one gave me something different. One said ‘use vinegar.’ Another said ‘don’t touch it.’ Third one gave me a wick and charged me $200. I’m just glad I didn’t lose my hearing. Australia’s healthcare system is a lottery.
So let me get this straight-you’re telling me the FDA approved a new ear drop that lasts 24 hours… and it’s called OtiRx? Sounds like a supplement sold on a YouTube ad. Who even names these things? ‘OtiRx’? Next they’ll release ‘CerebRx’ for brain fog and ‘GutRx’ for existential dread. At this point, I’m just waiting for ‘SleepRx’ that comes in a vape pen.
I had this bad case last winter. Didn’t even swim. Just showered and used a Q-tip. Ended up with a wick. It felt like a tiny sponge was trying to escape my ear. But yeah, it worked. The pain was unbearable-like someone was drilling into my skull. I didn’t realize how much I took my hearing for granted until I couldn’t hear my own breathing.
Don’t use peroxide. It burns. Just use the vinegar drops. Cheap, works, no drama. Also, dry your ears with a hair dryer on cool. It’s magic.
Have you considered that this entire narrative is manufactured by Big Pharma? The ‘acetic acid’ solution? It’s literally vinegar. Why isn’t it sold in grocery stores? Why do we need a ‘prescription’ for a substance that’s been in kitchens since Roman times? And why is Ciprodex $147.50? The active ingredients cost less than $2. This isn’t medicine-it’s a monopoly. The ‘fungal infection’ statistic? Likely inflated. The ‘94% effectiveness’? Probably funded by the manufacturer. The ear canal is not a battlefield. It’s a biological boundary. And we’re being sold war.
The philosophical underpinnings of otitis externa reveal a deeper epistemological crisis in contemporary medical paradigms: the reduction of biological complexity to pharmacological intervention. The ear canal, as a microcosm of homeostatic equilibrium, is not merely a conduit for sound but a sentient interface between organism and environment. To treat it with synthetic agents is to impose a Cartesian duality upon a holistic system-thereby exacerbating the very dissonance that precipitates the pathology. The true cure lies not in drops, but in ontological humility: to cease the violent interventionism of cotton swabs and embrace the ear’s innate capacity for self-regulation.
just wanted to say-i used the acetic acid drops after swimming for a year. zero infections. no drama. my 8-year-old does it too. it’s like brushing your teeth but for your ears. so simple. why do people make it so complicated? also, don’t be scared of the 5 minute wait. just lie there and watch a youtube video. it’s fine.
Did you know the government is using ear infections to track your location? The wicks? They have microchips. The drops? They contain nanobots that upload your browsing history. I had a doctor ask me about my phone usage right after I got the wick. Coincidence? I don’t think so. And why do all the studies come from the U.S.? Who funds them? Think about it.