 18
Mar,2026
18
Mar,2026
When you’re over 65, your body doesn’t just slow down - it changes how medicines work. A drug that was perfectly safe at 50 might cause dizziness, confusion, or even hospitalization at 75. Why? Because your liver and kidneys, the two main organs that process and remove drugs from your body, aren’t working like they used to. These changes aren’t minor. They’re powerful enough to turn a normal dose into a dangerous one. And yet, many doctors still prescribe the same pills the same way they would to a younger person. That’s where the real risk lies.
What Happens to Your Liver as You Age
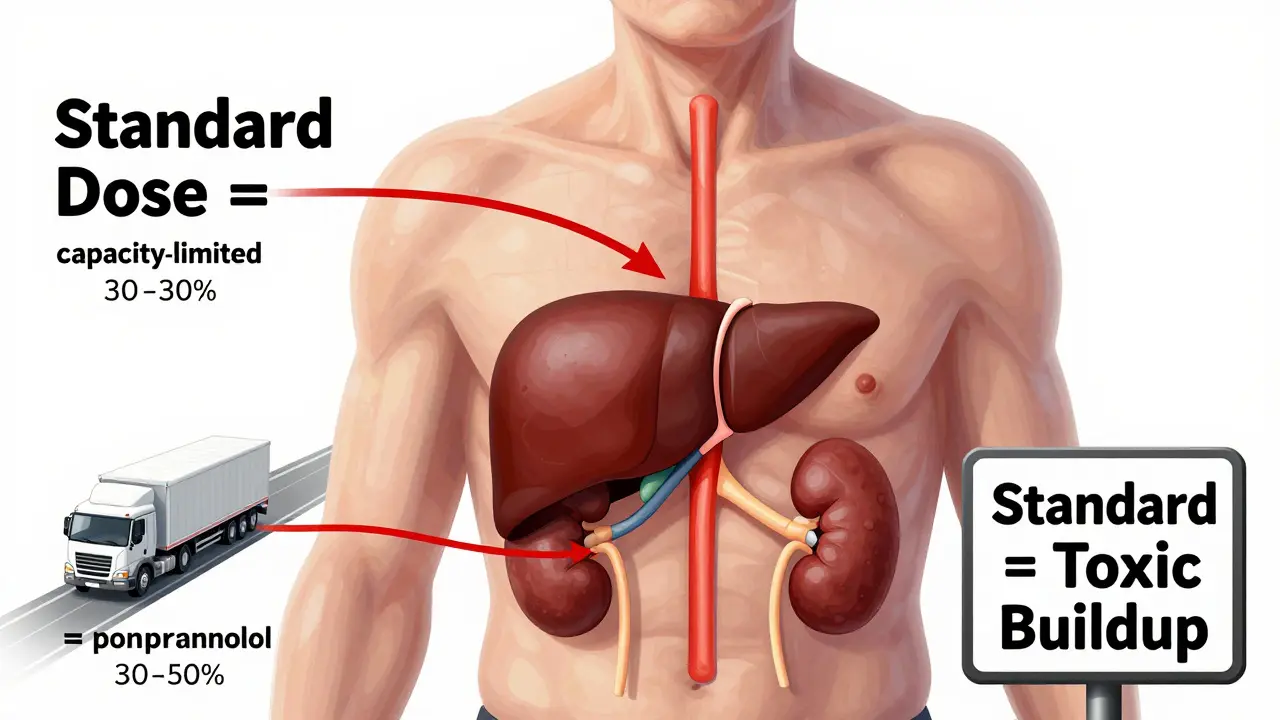
Your liver shrinks. Not a little - about 30% less mass by the time you’re 80. Blood flow to it drops by 40%. That means drugs don’t get processed as fast. For some medications, this sounds like a good thing: fewer side effects. But it’s not that simple. Think of your liver as a factory. Some drugs are like heavy trucks that need lots of fuel to move through - those are called flow-limited drugs. Examples include propranolol (for high blood pressure), lidocaine (a local anesthetic), and morphine (for pain). These drugs rely on blood flow to get into the liver and be broken down. When blood flow drops, clearance drops too - by about 40%. That means more of the drug stays in your bloodstream. Even a standard dose can build up to toxic levels. Then there are capacity-limited drugs, like diazepam (Valium), phenytoin (for seizures), and theophylline (for asthma). These don’t need much blood flow. Their breakdown depends more on enzyme activity. Here’s the surprising part: the enzymes that break these down - the cytochrome P450 family - don’t decline as much as you’d think. Some studies show only a 10-15% drop in their ability to process these drugs. So, while your liver is shrinking, it’s still doing a decent job with these. But here’s the catch: many older adults take multiple drugs. One might slow down the enzymes that break down another. Or, a drug like amitriptyline (used for depression or nerve pain) might be metabolized by an enzyme that’s already working slower. The result? A buildup that causes drowsiness, falls, or confusion. One Reddit user shared how their 82-year-old mother started on a standard dose of amitriptyline and became so dizzy she couldn’t walk. It wasn’t the dose itself - it was her liver’s reduced ability to clear it.Your Kidneys Don’t Just Slow Down - They Get Clogged
Your kidneys filter about 120-150 quarts of blood each day. By age 80, that drops to 60-80 quarts. That’s a 30-50% drop in glomerular filtration rate (GFR). But here’s the trap: doctors often look at serum creatinine to judge kidney function. And in older adults, creatinine stays normal because muscle mass declines. Less muscle = less creatinine. So your kidney function could be half of what it was, but the blood test looks fine. Drugs that leave the body mostly through the kidneys - like digoxin (for heart rhythm), lithium (for bipolar disorder), and many antibiotics - need lower doses. If you don’t adjust for reduced GFR, these drugs can accumulate. A 78-year-old patient on vancomycin (an antibiotic) nearly developed kidney failure because the dose wasn’t adjusted. Once doctors used the CKD-EPI equation (a more accurate way to estimate GFR without race-based corrections), they lowered the dose and avoided harm. And here’s something newer: kidney problems can actually hurt your liver’s ability to work too. Studies now show that when kidneys fail, liver enzymes like CYP3A4 become less active. So even if a drug is mainly cleared by the liver, poor kidney function can still cause it to build up. It’s a double hit.Prodrugs and First-Pass Metabolism: Hidden Risks
Some drugs aren’t active until your liver turns them into something else. These are called prodrugs. Perindopril (a blood pressure pill) is one. In younger people, the liver converts it quickly. In older adults? That conversion slows. The result? The drug doesn’t work as well. You might think it’s not helping - but the real issue is that your body isn’t turning it into the active form. On the flip side, drugs with high first-pass metabolism - like verapamil (for heart rhythm) or propranolol - get broken down heavily the first time they pass through the liver. When liver flow drops, less gets broken down. That means more of the drug enters your bloodstream. Bioavailability can jump by 25-50%. That’s why a 10 mg dose of propranolol in a 30-year-old might be fine - but in a 75-year-old, it’s equivalent to a 15-20 mg dose. No wonder some older adults feel faint or have slow heart rates after starting these meds.
How Many Medications Are Too Many?
It’s not just about one drug. It’s about how many you’re taking. The National Health and Nutrition Examination Survey (NHANES) found that 41% of adults over 65 were taking five or more prescription drugs. That’s not unusual. But each extra pill adds risk. Polypharmacy - using five or more medications - increases the chance of a hospital visit due to an adverse drug reaction by 88%. And it’s not just interactions between pills. Over-the-counter drugs matter too. Acetaminophen (Tylenol) is the leading cause of acute liver failure in older adults. Why? Because liver enzymes are slower, and people often take it daily for arthritis pain, not realizing the cumulative effect. The Beers Criteria® - a guide used by geriatric pharmacists - says: start low, go slow. For drugs mainly cleared by the liver, reduce the starting dose by 20-40% for people over 65. For those over 75, go even lower. Don’t assume your body handles things like it did in your 40s.What Should You Do?
If you’re over 65 and on multiple medications, here’s what to ask your doctor:- Which of my drugs are cleared by the liver? Which by the kidneys?
- Have you checked my kidney function with the CKD-EPI equation, not just creatinine?
- Could any of these be prodrugs that need more time to work?
- Am I on any drugs that are on the Beers Criteria list for older adults?
- Could we try reducing one drug at a time to see if symptoms improve?

What’s Changing in 2026
The FDA now requires drug trials to include more older adults - but only 38% of participants in new drug studies are over 65. That means we still don’t know how many new drugs behave in aging bodies. A new tool called GeroDose v2.1, approved in 2023, lets doctors input age, weight, liver enzymes, and kidney function to simulate how a drug will behave in a specific person. It’s not perfect - but it’s a step toward personalized dosing. Researchers are also looking at epigenetics - how genes turn on and off with age. A 2023 study found 17 methylation sites linked to CYP3A4 activity that change as we get older. This could one day help predict who’s at risk for bad reactions before they even start a drug.The Bottom Line
Age isn’t just a number. It’s a physiological shift. Your liver and kidneys aren’t broken - they’re just different. But that difference can turn a safe medicine into a dangerous one. The fix isn’t stopping meds. It’s adjusting them. Start with lower doses. Monitor kidney and liver function properly. Cut out unnecessary pills. Ask questions. Because when it comes to medications in older adults, the right dose isn’t about what’s on the label - it’s about what your body can handle today.Why do older adults need lower doses of some medications?
Older adults need lower doses because their liver and kidneys don’t process drugs as efficiently. Liver blood flow drops by 40%, liver mass shrinks by 30%, and kidney filtration (GFR) declines by 30-50%. This means drugs stay in the body longer, increasing the risk of side effects. Even if blood tests look normal, organ function has slowed - so standard adult doses can become toxic.
Can a normal creatinine level mean poor kidney function in seniors?
Yes. Creatinine is made by muscle. As people age, they lose muscle mass - so even if kidneys are working at half capacity, creatinine levels can appear normal. That’s why doctors should use the CKD-EPI equation to estimate glomerular filtration rate (GFR), not just rely on creatinine. Ignoring this can lead to dangerous overdoses of kidney-cleared drugs like digoxin or antibiotics.
Are over-the-counter drugs risky for older adults?
Absolutely. Acetaminophen (Tylenol) is the leading cause of acute liver failure in older adults because it’s taken daily for pain, and the liver can’t clear it effectively. NSAIDs like ibuprofen can worsen kidney function and raise blood pressure. Even herbal supplements like St. John’s Wort can interfere with prescription drugs. Always tell your doctor what you’re taking - even if it’s "just a vitamin."
What’s the difference between flow-limited and capacity-limited drugs?
Flow-limited drugs (like morphine, lidocaine, propranolol) depend on blood flow to the liver to be cleared. When liver blood flow drops with age, these drugs build up fast. Capacity-limited drugs (like diazepam, phenytoin) depend on enzyme activity. Those enzymes change less with age, so clearance drops only slightly. Knowing which category a drug falls into helps predict how much to reduce the dose.
How do you know if a drug is a prodrug?
A prodrug is inactive until the liver converts it. Common examples include perindopril (blood pressure), codeine (pain), and clopidogrel (blood thinner). In older adults, this conversion slows, so the drug may not work as well. If you’re on one of these and notice reduced effect, it could be due to slower liver metabolism - not because the drug isn’t working, but because your body isn’t turning it into its active form.
Is polypharmacy really that dangerous for seniors?
Yes. Taking five or more medications increases the risk of hospitalization from adverse drug reactions by 88%. Each extra pill adds interaction risk. One drug might slow liver enzymes, causing another to build up. Another might affect kidney clearance. The more drugs, the harder it is to predict how they’ll behave together - especially with aging organs.
What tools are doctors using today to adjust doses for older patients?
Doctors use the Cockcroft-Gault and CKD-EPI equations to estimate kidney function. For liver metabolism, they follow the Beers Criteria®, which recommends starting doses 20-40% lower for seniors. New tools like GeroDose v2.1 (FDA-approved in 2023) simulate drug levels based on age, weight, liver enzymes, and kidney function - helping tailor doses more precisely than ever before.



Oh wow, so now we're just supposed to trust that doctors know what they're doing? 🤡 My grandma took 14 meds and still thought she was 30. Then she fell, broke her hip, and the hospital said 'you're lucky you're alive.' Guess what? The 'standard dose' was literally poison for her liver. And no one checked her kidney function. They just kept adding more pills because 'it's what we've always done.' Welcome to healthcare, folks. It's not broken. It's designed to profit off your decline.
I'm so heartbroken 😭 that our elders are being poisoned by the very system meant to help them. I cried when I read this. My dad almost died from Tylenol because he took it every day for his back pain. No one told him. No one asked. Just 'take two for pain.' We need to treat our seniors like humans, not numbers. Please, if you're reading this, talk to your parents. Ask them what meds they're on. Don't wait until it's too late.
There's a quiet revolution happening in geriatric pharmacology-one that doesn't make headlines but saves lives every day. The shift from population-based dosing to physiological reality is long overdue. The liver isn't 'failing' with age; it's adapting. And so are we. When we stop treating aging as a disease and start treating it as a physiological state, we begin to see the elegance of dose adjustment. It's not about reducing medication-it's about honoring the body's changing capacity. This post isn't just informative. It's a call to reframe how we think about care.
The data presented here is compelling and aligns with clinical guidelines established over the past two decades. It is imperative that prescribing practices evolve to reflect the physiological changes associated with aging. The reliance on serum creatinine alone is a persistent error in clinical reasoning. The adoption of CKD-EPI and GeroDose tools represents a necessary step toward precision medicine. I commend the author for highlighting the intersection of pharmacokinetics and geriatric vulnerability.
You know what they don't tell you? The pharmaceutical industry knew this for decades. They just kept pushing 'standard doses' because older people are more profitable. They don't care if you're dizzy. They care if you're buying more pills next month. And don't get me started on 'over-the-counter' drugs-those are just gateway drugs for the next prescription. Your 'Tylenol' is a Trojan horse. The FDA? They're in bed with Big Pharma. Wake up.
This is deeply important. In India, many elderly take medications without any monitoring. Family members assume the doctor knows best. But here, the system doesn't even test kidney function properly. We need community health workers to educate families-not just doctors. A simple conversation about liver and kidney changes could prevent so much suffering. I have seen it. My aunt nearly lost her kidneys because of an antibiotic. We didn't know. Now I teach others.
Wait...wait...WAIT... So you're telling me that the government, the FDA, the AMA, and Big Pharma are all hiding this? That they've been poisoning our grandparents for decades? And now they're using 'GeroDose' like some kind of magic solution? That's just a distraction! The real truth? It's all about control. They want you dependent. They want you scared. They want you to keep taking pills. And now they're using science to make it look legit. This is a mind control program disguised as medicine. I've been researching this for 12 years. They're not fixing the system-they're monetizing the breakdown.
The Beers Criteria is a necessary framework, but its implementation remains inconsistent across primary care settings. In my practice, I have observed that physicians frequently overlook prodrug metabolism, particularly in patients with polypharmacy. Furthermore, the assumption that reduced muscle mass equates to reduced drug clearance is not universally understood. I strongly recommend mandatory geriatric pharmacology modules in residency training. Without structural education reform, even the best guidelines remain theoretical.
This is spot on. I've been a pharmacist for 22 years. I've seen too many seniors admitted for toxicity from drugs that were never adjusted. The worst? When the family says, 'But the doctor said it was fine.' No, they didn't. They just clicked 'confirm' in the EHR. I always ask: 'What's your creatinine? What's your eGFR? Are you on a prodrug?' If the answer is 'I don't know,' I slow down the whole regimen. One drug at a time. Always. And yes-Tylenol is the silent killer. It's not the dose. It's the frequency.
I'm 71 and on five meds. I read this and finally understood why I felt so foggy after starting that new painkiller. My doctor didn't explain any of this. Just said 'take one.' I stopped it. Waited a week. Felt better. Now I ask questions. I tell my kids what I'm on. It's not about being difficult. It's about being alive. You don't need to be a doctor to know your body. You just need to care enough to ask.